Can you sit down on the floor and stand back up—without using your hands, knees, or any other support?
It sounds like a party trick. But in a landmark study of over 2,000 adults, those who couldn't do it had roughly 5 times the mortality risk compared to those who could1. Only 2 of 159 deaths during follow-up occurred in people with a perfect score1.
That's a sobering finding. But like the 10-second one-leg balance test, it's also a hopeful one—because the skills this test measures (strength, flexibility, balance, coordination) are all trainable at any age.
This article is for education, not medical advice. If you have joint replacements, significant knee or hip pain, recent surgery, or a history of falls, talk with your clinician before trying this test.
Quick Take
- What it is: Sit down on the floor and stand back up, using as little support as possible. Score out of 10.
- Why it matters: In a 2012 study, adults (ages 51-80) who scored 0-3 had roughly 5 times higher mortality over ~6 years compared to those scoring 8-101.
- What it measures: Musculoskeletal fitness—strength, flexibility, balance, and motor coordination working together.
- What it does not mean: A low score doesn't diagnose a disease or predict your personal outcome. It's a signal, not a sentence.
- What to do with it: Treat it as a starting point for targeted training.
What Is the Sitting-Rising Test?
The sitting-rising test (SRT) was developed in the 1990s by Brazilian physician and exercise researcher Dr. Claudio Gil Araújo at the Clinimex exercise medicine clinic in Rio de Janeiro1. He needed a quick, equipment-free way to assess his patients' overall musculoskeletal fitness—the kind of whole-body functional ability that aerobic tests like treadmill runs don't capture.
The concept is deceptively simple: from a standing position, lower yourself to a seated position on the floor, then rise back to standing. The less support you need, the higher your score.
What makes the SRT powerful is that it challenges multiple fitness components at once:
- Muscle strength and power (especially legs and core)
- Flexibility (hips, knees, ankles)
- Balance and coordination (controlling your center of gravity through a large range of motion)
- Body composition (carrying extra weight makes the movement harder)
These are the same abilities that predict whether someone can live independently, recover from illness, and avoid falls. (For the deeper science on how balance works, see 6 Body Systems Critical for Balance.)
The Study Behind the Headlines
In 2012, Araújo and colleagues published a study in the European Journal of Preventive Cardiology that followed 2,002 adults ages 51-80 for a median of 6.3 years1.
Each person performed the SRT and received a composite score from 0 to 10. During follow-up, 159 deaths occurred (7.9% of the group)1.
The results were striking:
| SRT Score Range | Adjusted Hazard Ratio | Meaning |
|---|---|---|
| 8-10 (little or no support) | 1.0 (reference) | Lowest mortality risk |
| 6-7.5 | 1.84 | ~2x higher risk |
| 3.5-5.5 | 3.44 | ~3.5x higher risk |
| 0-3 (needed significant support) | 5.44 | ~5.4x higher risk |
These hazard ratios were adjusted for age, sex, and body mass index—meaning the relationship held even after accounting for those factors1.
Another way to read the data: each 1-point increase in SRT score was associated with a 21% improvement in survival1.
Why does sitting and standing predict survival?
The SRT isn't magic. It's a composite measure of the physical capabilities that keep you functional and resilient:
- Leg strength to push yourself up
- Core stability to control the movement
- Flexibility to get into and out of a deep position
- Balance to stay steady through a wide range of motion
- Coordination to sequence the whole movement smoothly
These are the same systems that help you catch yourself when you trip, climb stairs, get off the toilet, and recover from illness or surgery. When they decline, independence follows. (For more on why these systems change with age, see Understanding Why Balance Declines with Age.)
How to Do the Test Safely at Home
Safety first
This test involves getting to the floor and back up. That's a real physical challenge for many people—and that's the point. But safety always comes first.
Do NOT attempt this test if:
- You have a joint replacement (hip or knee) with movement restrictions
- You have significant knee, hip, or back pain
- You've had recent surgery
- You have severe balance problems or a history of falls
- You feel dizzy or lightheaded
If you're unsure, try it with a spotter—someone standing nearby who can offer a hand if you get stuck.
Setup
- Clear space: At least 6 feet by 6 feet of open floor, no furniture edges to bump into.
- Surface: Firm, non-slip floor. No thick rugs or slippery surfaces.
- Clothing: Comfortable clothes that don't restrict movement. Bare feet (or non-slip socks).
- Optional: Place a yoga mat or thin cushion on the floor for knee comfort—but keep it flat and stable.
The test protocol
Part 1: Sitting down (5 points possible)
- Stand tall, feet roughly shoulder-width apart.
- Without using any support, lower yourself to a cross-legged seated position on the floor.
- Try not to use your hands, knees, forearms, or the side of your leg for support.
Part 2: Rising up (5 points possible)
- From the seated position, rise back to standing.
- Again, try to use as little support as possible.
You can try multiple times. If your first attempt is shaky, rest and try again. Your best score counts2.
How to score yourself
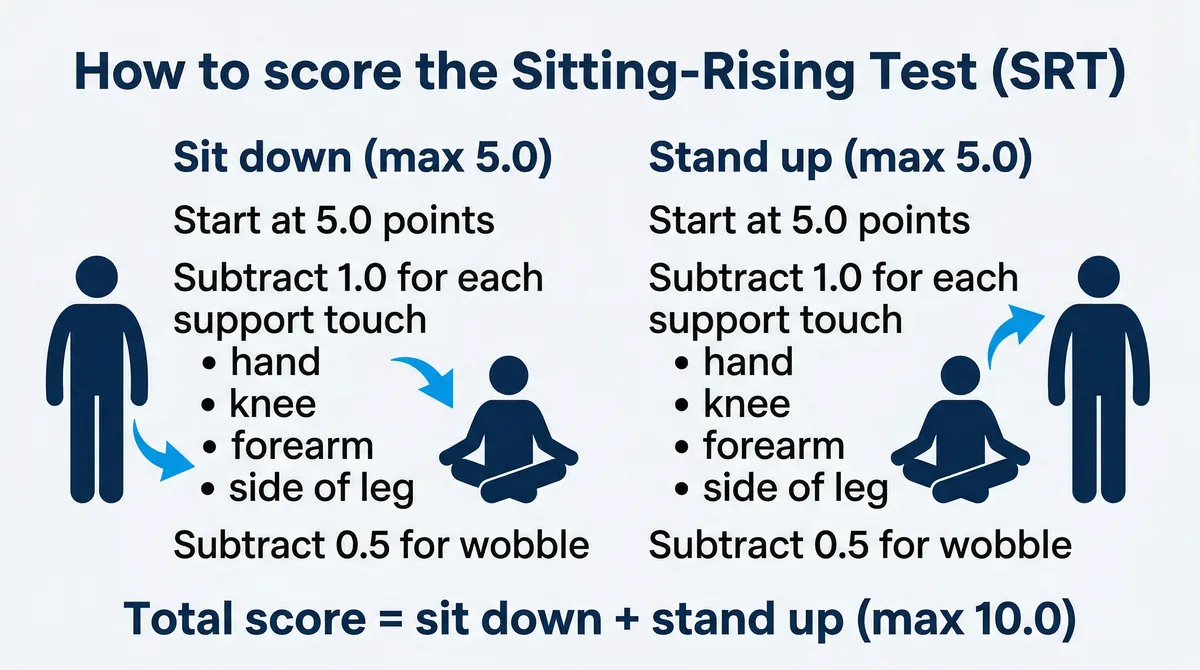
Start with 5 points for sitting and 5 points for rising (10 total).
Subtract 1 point each time you use:
- A hand on the floor
- A hand on your knee
- A forearm on the floor
- A knee on the floor
- The side of your leg for support
Subtract 0.5 points for:
- Noticeable unsteadiness or partial loss of balance during either movement2
| Score | What it means |
|---|---|
| 8-10 | Excellent. Little or no support needed. |
| 6-7.5 | Good. Minor supports used. Room to improve. |
| 3.5-5.5 | Fair. Multiple supports needed. Training recommended. |
| 0-3 | Needs attention. Significant support required. Talk to a clinician. |
How to Interpret Your Score
If you scored 8-10
Strong work. You have good musculoskeletal fitness for this movement. Don't stop—keep investing in the strength, flexibility, and balance that got you here.
Next steps:
- Challenge yourself with balance training: The Complete Guide to Balance Training for Seniors
- Check other dimensions of your balance with Simple Balance Tests You Can Do at Home
If you scored 3.5-7.5
You're in the middle—and that's a useful place to be. You have room for meaningful improvement, and the research suggests that every single point matters (21% survival improvement per point)1.
Next steps:
- Start the improvement plan below.
- Focus on the specific limitation: Was it strength (couldn't push up), flexibility (couldn't fold into the position), or balance (wobbled or tipped)?
If you scored 0-3
This is important information, not a verdict. Many people in this range can improve significantly with targeted training.
Next steps:
- Talk to your doctor or a physical therapist. A low SRT score often overlaps with other fall risk factors worth investigating.
- Begin with supported exercises (see plan below).
- Don't rush to re-test. Focus on building strength and confidence over weeks.
If you couldn't attempt the test at all
That's still valuable data. It means prioritizing functional fitness—especially getting up and down from the floor safely—should be near the top of your health to-do list.
What This Test Adds Beyond the 10-Second Balance Test
If you've already tried the 10-second one-leg balance test, you might wonder what the SRT adds. They're complementary:
| 10-Second Balance Test | Sitting-Rising Test | |
|---|---|---|
| Primary focus | Static balance and postural control | Whole-body functional fitness |
| Key systems tested | Vestibular, vision, proprioception | Strength, flexibility, balance, coordination |
| Movement | Stand still on one leg | Full sit-to-stand transition |
| Equipment | None (counter nearby for safety) | None (clear floor space) |
| Study population | Ages 51-753 | Ages 51-801 |
Together, they give you a more complete picture of your physical resilience. The balance test asks: Can you hold steady? The SRT asks: Can you move your whole body through a challenging range of motion?
A 4-Week Plan to Improve Your Score
The good news: every component the SRT measures responds to training. Here's a progressive plan.
Week 1-2: Build the foundation (5-10 minutes/day)
Leg strength:
- Chair squats: Stand in front of a sturdy chair. Lower yourself until you lightly touch the seat, then stand back up. 3 sets of 8-10 reps.
- Wall sits: Back flat against a wall, slide down until knees are at ~90 degrees. Hold 15-30 seconds. 3 rounds.
Flexibility:
- Hip circles: Stand near a counter. Swing one leg in small circles. 10 each direction, each leg.
- Seated hip stretch: Sit on the edge of a chair. Cross one ankle over the opposite knee. Lean gently forward. Hold 20-30 seconds per side.
Balance:
- Supported single-leg stands: Hold a counter, lift one foot. Hold 15-20 seconds, 3 rounds per side. (See our complete balance training guide for progressions.)
Week 3-4: Practice the movement (add to above)
Floor transition practice (with support):
- Stand next to a sturdy piece of furniture (couch arm, heavy chair).
- Use the furniture as much as you need to lower yourself to the floor.
- Sit for a moment. Then use the furniture to help yourself back up.
- Each session, try using the furniture a little less.
- 3-5 rounds, resting as needed.
Core work:
- Dead bug: Lie on your back, arms up, knees bent. Slowly extend one arm and the opposite leg. Alternate sides. 3 sets of 8 per side.
Re-test after 4 weeks. Most people who train consistently can gain 1-3 points. Research on exercise programs for older adults confirms that targeted strength and balance training can meaningfully improve stability and functional capacity4.
FAQs
Is this test safe for everyone?
No. People with joint replacements, significant joint pain, severe balance disorders, or recent surgery should skip it or get clearance from a healthcare provider first. If you can't safely get to the floor and back up, that information alone is worth discussing with your clinician.
Does age affect what's a "good" score?
Yes. A 2020 follow-up study established age- and sex-specific reference values for over 6,000 adults2. Scores naturally decline with age—a 70-year-old and a 50-year-old shouldn't expect the same number. What matters most is whether your score is in a healthy range for your age and whether it's improving over time.
I have bad knees. Does that invalidate the test?
Not entirely, but it changes the context. The SRT measures overall musculoskeletal fitness, and knee issues are part of that picture. If you lose points because of knee pain or stiffness (rather than weakness or balance), note that and focus on what's within your control—hip mobility, core strength, and upper-body support patterns.
How often should I re-test?
Every 4-8 weeks is reasonable if you're actively training. More frequent testing doesn't help—the changes happen gradually.
Does body weight affect the score?
Yes. The SRT is harder for heavier individuals because you're lifting and lowering more weight through a large range of motion. In the original study, BMI was one of the factors they adjusted for—and the mortality association still held1. That said, carrying extra weight doesn't disqualify you. Improving strength and flexibility at your current weight still improves your score and your functional fitness.
What if I can sit down fine but can't get up?
That pattern is common and points specifically to leg strength and power as the bottleneck. Chair squats, wall sits, and stair-step exercises are your highest-value investments.
Want to Track Your Progress?
The SRT gives you a snapshot. But lasting improvement comes from consistent practice and measurement over time.
One point at a time. That's how functional fitness is built.


